One of my closest friends, Nancy, who I lived with for my final year of university, has a certain saying. She is far from a philosophical girl, but when something didn’t go according to plan, she’d just shrug and say “It is what it is”. Although this acceptance was usually in reaction to using the last of the toilet paper, having a filthy room, or uncertainties about what would happen upon finishing our degrees, it is an attitude that I’ve been striving to adopt recently.
As I said, Nancy never considered a life threatening situation during these shrugging moments, but the simplicity of her words and her understanding of the fact that some things are just beyond your control, and that you must just make do with whatever those things are, remain good guidelines to live by.
I cannot believe it has been nearly a month since I last posted. So much has happened. I hate the words ‘journey’, and ‘battle’. I hate equating cancer to some kind of war. Because although there are lab technicians squinting at my blood and consultants using my cell counts to come up with a plan of attack, and scientists mixing up chemicals into bags with my name on in order to, hopefully, blow some of these cells away, this doesn’t feel like a battle. A battle implies excitement, action, shouting, running. The reality involves a lot more waiting, hushed words, time spent staring at the ceiling. Perhaps occasional, ashamed tears whispering onto a nurse’s uniform behind a curtain. I would describe it as more of a slog, than a battle. That said, I have been on a journey or two, somewhat. Thankfully, they’ve mostly been physical ones, instead of head-spinning mental quests to find myself.
For those who don’t know, my doctors chose Option 2. After I posted my last spiel about blood results and chemo and maybe-dying, I headed back to see my doctor, and he told me that they’d chosen the route I hoped for: another strong round of chemo, a couple of weeks for my body to recover, and then straight into my pre-transplant chemo. As discussed, this is the route that will cause my body a bit more grief, but may also give me what is, essentially, a longer life expectancy (words that make me shudder to type. There are some things that you can never adjust to). So I went straight back into hospital for chemo round 3, a new combination of drugs, thankfully lasting less than a week, and I reacted pretty well to them. I experienced a few temperatures that were pushing 40 degrees, a lot of night sweats, and a complete lack of appetite, but no sleepwalking, hallucinations, or 5am ice baths. I’m pretty sure all of the nurses were as glad about this as I was, despite eyeballing me and my fevers more strictly this time. A couple of nurses have reminded me in these last couple of weeks that I’m a rare and interesting case, but this was highlighted a lot more when I had five medical students come in and try and guess my diagnosis through my symptoms. They’d never heard of MDS, or of my treatment plan. On top of that, on the first day of my chemo, I asked my doctor how long one of the bags of drugs ran for, and he wasn’t sure. Several doctors seemed a bit nonplussed, and had to go and look it up, as that drug was so rarely used. I think some of the newer staff members had never seen it on the ward before, which was a bit unnerving.
A couple of nurses have reminded me in these last couple of weeks that I’m a rare and interesting case, but this was highlighted a lot more when I had five medical students come in and try and guess my diagnosis through my symptoms. They’d never heard of MDS, or of my treatment plan. On top of that, on the first day of my chemo, I asked my doctor how long one of the bags of drugs ran for, and he wasn’t sure. Several doctors seemed a bit nonplussed, and had to go and look it up, as that drug was so rarely used. I think some of the newer staff members had never seen it on the ward before, which was a bit unnerving.
My physical journeys involved trips to the lung function unit and the cardiology department for a few pre-transplant workups. These were pretty simple, but I was fuming to find out that my lung function was poorer than I expected. It was distinctly average, but I protested violently that I had expected to be above average (you know me, I like to win and stuff). I guess that a decade of pretending to forget my gym kit so that I didn’t have to do hockey at school, and then wasting money on a uni gym membership card that grew dusty in a drawer have caught up with me.
In between these tests, I found time to post my dissertation and other uni work off on a physical journey, too. As thrilled as I am to turn these in to the English Department in Cardiff and never have to see them again, a couple of nurses seem to have made it their mission to keep me entertained within the confines of my hospital cell, which is entertaining in itself. One brought in a game that she plays with her six year old niece, which, embarrassingly, is bloody hard.
Celebrating my final hand-in, albeit not as I expected to!
I’m finally brain-training my restless body into filling up my free time. I try to spend less time staring at the wall with my headphones in, but have progressed to reading kids books and embarrassingly simple chick lit. My fuzzy brain hasn’t been able to focus on a lot else.
Following chemo and a week of crossed fingers, my doctors let me out to celebrate my 21st birthday at home, and my friends and I had a lovely day with a lot of cake, and, in my case, even more champagne.
I was mercilessly teased when I returned to the ward that night with a burning fever that made me shiver, and an early-onset hangover. Luckily, the night doctor quickly shoved a glucose and fluid drip in my arm and I woke up feeling more embarrassed than I did headache-y. On the plus side, I would definitely recommend such drips to a friend with an approaching 9am lecture, and it was brilliant to have a day off from being a cancer patient.
After the sugary, bubbly high of my birthday, I spent last week on a bit of a harsh comedown to reality. On Tuesday, my consultant said he wanted to pop in “for a chat”. By now, I should’ve learnt that a ‘chat’ with a consultant is never just a catch-up to see how you’re doing, but often something more serious. But I remained naive until he turned up in my cell armed with a stack of paperwork, a transplant specialist nurse and a grim expression. It was time, it seemed, to do what I’d been putting off, and talk through the transplant paperwork.
You may remember the German donor they found for me back in November, whose stem cells were a 90% match to mine. As positive as it sounds, this is in fact the lowest percentage match they’ll use for a transplant. If your cells are too different, the donor cells won’t stand a chance. Your body will completely reject them, and you could get pretty ill very quickly. We held out hope for a 100% match coming along, but due to my rare gene typing (because my body hasn’t given me enough problems as it is, thank you to me), one hasn’t surfaced. As we’re running out of time now, it’s time to go ahead with this German donor, and I’ve got a decent chance of a 90% match being successful.
We sat down and talked through chemo regimes, immunosuppression drugs, chances of success and failure, side effects, and then he hesitated and asked if I wanted to “talk numbers”. This is not your typical dodgy business deal, as I may be making it sound, but the statistics about my long term survival. Even better. As I’m sure you may remember, they’re not great, but I smiled and nodded through the signing of the papers, and then I signed my name at the bottom of this piece of paper. I signed my agreement to a procedure that involved a 20% risk of death within the first few weeks, because I’ve finally reached the point where agreeing to anything that doesn’t have even a small risk of death appears dull. Unfortunately, what I was signing my name to was also the possibility of feeling horrendous and still having an 80% chance of the cancer coming back in the next couple of years.
A couple of friends visited, I forgot about the paperwork, and it was only later, curled up in the cell, with my dad visiting, that the combination of the pain from an infection, the impact of the paperwork that day, and the army of nurses who’d asked me if I was ok or if I needed to talk about my former ‘chat’ finally hit me. My friends and I had spoken earlier, as we so often do, of how long we’ve been friends for, how lucky we are, where we may all be in five years’ time. It’s becoming increasingly harder to accept that I may not even be around in five years. It hits me at random moments. When I’m in bed suffering a horrendous chemo night-sweat, and wondering if all this is worth it, when I’m lucky enough to come home for the day and I’m sitting in my garden appreciating the silence, when I’m wasting my time on a particularly crap book. Or, as is more common, when my friends are discussing the future, and, for the first time, I have nothing to contribute to the conversation. Cancer often means that you have no idea where you’ll be or how you’ll be feeling in five hours, five days. Let alone five years.
But, as Nancy would say, it is what it is. This is the situation I’ve found myself in. It may be far from ideal, but what choice do I have but to sign the paperwork, sit back, and accept more drugs? Because if I didn’t believe that my life was worth fighting, or slogging, for, then I wouldn’t still be here today.
On Wednesday, the line team turned up to have a fiddle about with the tubes currently crisscrossing around my veins. I’ve had my PICC line in since February, and loved it. It’s made my life so much easier, and minimised the amount of nervous sweats over needles and cannula kits. But now, my poor little PICC line isn’t strong enough to cope with the amount of drugs and transfusions I’ll need during my transplant. It was time for a Hickman line, a bigger, multi-tubed line inserted through my neck, and tunnelling into the vein by my heart. I was told that the insertion of it would take no longer than about 20 minutes, with some local anaesthetic and sedation if I needed it. After dutifully starving myself all morning, the team turned up at half 11 to put it in, and within a couple of minutes, I had three specialist nurses fussing around me, sending my mum out of the room, and I found myself lying back with an oxygen mask, holding my nurse’s hand. She had tactfully chosen the hour before the line team arrived to tell me that she fainted the first time she’d seen a Hickman line inserted, which didn’t help my twitchiness, but she insisted on staying with me, and I’m pleased that I had someone with me this time.
They tried out a bit of sedation on me, and, just before they were about to start the prodding around, I asked for more. Thankfully, they dosed me right up to oblivion, because it was apparently a pretty tricky job. The 20 minute procedure took over an hour, as the vein in my chest kept collapsing, exhausted after three intense rounds of chemo, and I was awake and apparently in pain, none of which I remember, because the main side effect of my sedative drug was a loss of ability to create new memories. I woke up five hours later, with my mum by my side, a sore chest and feeling too groggy and sleepy to even read a caption on my Instagram feed, which was arguably the most disappointing part of the whole experience. I’m thrilled not to remember any of what sounds like a fairly gruesome experience. Plus, my sore chest is slowly getting better, despite now having boobs full of tubes. Tubes which need taping up the whole time. For a few days, there were five tubes hanging in and out of my chest and arm, but my PICC has now been pulled out, so I’m down to three. 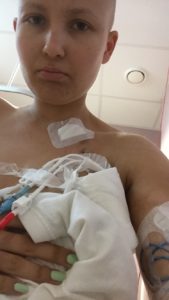
On Thursday, the fourth day of my Diary of Doom, the doctors turned up and told me that they could fit me in for a biopsy that morning. There was initially some doubt as to whether I should have one at all: if my chemo hadn’t worked again, wouldn’t I feel more miserable going into the transplant knowing that? Wouldn’t it be better to just hope for the best? I wasn’t capable of this kind of guesswork, however. I just had to know. I pushed for a biopsy (for the first and last time, I imagine), and I got one, which two nurses held my hand through, and we managed, because we had to. It is what it is, after all.
On Saturday, another doctor kept me nervously pacing the floor waiting for the results, and when he turned up he told us that my biopsy did show some evidence of success: the chemo I’ve just had has had a small impact on the number of cancer cells in my bone marrow. I felt that I should be thrilled, relieved, but I felt a bit empty. I think I’m so used to preparing myself for the worst news now, that I didn’t even know how to react to this good news. But I think the most disappointing thing about this chemo was that it hadn’t done what I’d dared to secretly hope. It hadn’t just dramatically reduced my cancer, or improved my chances. It ups the chances of my transplant working, and of me surviving, long-term, without cancer, by about 5%.
And that’s ok, really, isn’t it? It’s better than bad news. I should be happy, shouldn’t I? But maybe being 5% better sometime in the future or maybe not, after the last week of poison, doesn’t sound like much, which is why I’m disappointed. Despite this really terrible week, the growing inevitability of my transplant has made me realise, more than ever, how much I really don’t want to die. But trying to live positively, and living whilst ignoring the odds, is exhausting. Once before, I wrote that positivity can be more exhausting than chemo, and I stand by that in the face of that terrible week.
Even my consultant knew it wasn’t really what I wanted to hear, however he packaged it. Even he looked me in the eye and said “It is what it is”. And I knew, then, that I had no choice but to carry on, and just make do with the shitty odds I’d been given.
Anyway, it’s a new week, my muddled chemo brain is starting to recuperate despite the fact that I start chemo again on Wednesday. This Wednesday. I’m not sure I’m ready for a fourth round so soon, or for a transplant in exactly ten days from now. But I’ll make myself ready. I will. Because what else can I do? Life is what it is, after all.





Hi Alice
I thought you may be interested in something I heard at the weekend. I was listening to BBC 5 live (sadly my favourite radio station, as I love all the chat). I had missed the beginning of a story and came in to a woman who was saying that 30 years previously she and her husband had decided (don’t know why, missed that bit) to sign onto the bone marrow donor list and then gone on with their lives. She then got a phone call, yes 30 years later, saying she was a 100% match to a man in America. She duly went through the process and over the next two years, when as I’m sure you know anonymity must be maintained, she swapped postcards and brief letters with the American. The story then goes to New York where a policeman who had been feeling unwell went for tests where the doctors said he had contracted leukaemia. It appears that he was part of the rescue services at 9/11 and that a number of people in his position had gotten ill from the effects of the dust!! He went through one round of Chemo and after a year was just about to get the all clear and return to work when he found out the cancer had returned. They discovered that this lady in England was a 100% match and after treatment he is still all well and good now. It was very touching to hear that they met after she had been invited to New York for a donor dinner. How lovely is that story? Just thought at this time you may like to hear uplifting stories. Stay strong Alice you are so well loved and mean so much to so many people. All the best Jane xx
Hi Alice
I read all of your posts and am totally inspired by your strength. Lucy keeps me up to date as you are doing and how tough if has been for you. Good luck over the next few weeks and I will be thinking of you.
You are amazing
Michelle x
Hi Alice,
I think instead of ‘it is what it is’ your blog should be ‘ you are who you are’ . You are so amazing how you are coping with all you’re going through fighting this horrible illness. You really are so inspirational and strong.It sounds like you have an amazing team of doctors and nurses around you too. We are all thinking of you xxx
Oh Alice you are amazing writing your blog when no doubt you feel absolutely awful with the cocktail of drugs they are giving you so pleased you managed to celebrate your 21st in between! Good news that there was some improvement after the last chemo you have turned corner! You wait til you get those German cells they will give this ghastly cancer a rude shock!!! We will be thinking of you as you go through the next hurdle lots of hugs Marian Sutherby
Dear Alice,
There is nothing and I mean nothing average about you. ‘You are what you are’ an incredibly strong, talented and loved friend and daughter who inspires and shows us what true grit is all about. Keep slogging and know that we sent our love and will be thinking of you as you face this next challenge xx
Hi Alice, I am Lucia and Bella’s cousin and I read your blogs when they share them on FB. I work for a company called Bristol Myers Squibb who have a number of oncology drugs in their portfolio. One of the internal campaigns we have running in the company is the ‘who do you work for?’ campaign. I can honestly say I work for people like you. You are one of my heroes and I’ve not even met you! Keep fighting the good fight. I know you have a great team of people on your side! Wishing you all the best and good luck with the next phase of your treatment xx
Hello Alice, hopefully you might remember me, I’m your mum’s cousin Alison, we last saw you at my son’s 1st birthday party and that was nearly 10 years ago!! and he’s going off to senior this September! Your Aunty Soph has been sharing your blogs..I’m so sorry this is happening to you, you are such an inspirational and strong young lady…all the best for the next challenge..my family and I are all thinking of you, all my love Alison xx
Hi Alice, completely echo your sentiments re battles and fights, but whatever the minutes hours and days are called you have an army of support behind you , think of you often- can’t tell you how truly awe inspiring your blogs are. Huge cyber hugs to you and all your family, xxxx
Hi there Alice – boy have you had some week!!! I have three friends who have gone through this stemcell transplant – my youngest son’s mother-in-law in California, Gea, and she’s just had a gall-bladder removed due to mothing to do with her cancer, and is doing brilliantly PTL – and Vicky here in Linlithgow just after Gea in CA, and she’s just amazing; and my sisterhood friend Olivia, who only lasted a year after hers – and two of her boys visited me this evening strangely enough! So have been through it second-hand a few times – 2 out of 3 aint bad odds in the cancer-world methinks!
Are you happy for me to continue praying for you as i did for my three friends Alice? And praying for all of you – body, soul and spirit? You certainly seem to have a great spirit! !
Many Blessings for Wednesday, i’ve a free day from praying for my Grandson Matthew’s exams that day, so you will get the full force of all the Blessings i can muster – much love, patricia – Jane Chapman’s Mother-in-law and she’s Mother of Matthew our gorgeous Grandson xxx
Praying for your chemo today Alice – right now here in my bed – asking my Best Friend Jesus to Use this aweful cell-killing medication to start up His Amazing Healing of your body, and to give you such a feeling of something special happening within you – asking too for you to start noting Amazing Blessings surrounding you today and tomorrow and every, yes EVERY day until you are completely Healed of this nasty invasive disease and are fully well again – praying for His Love to come to you today thru The Blessings He will Send to you – watch out for them – some will be so unexpected and others will find you warmed by His Own dear Presence – dear Alice ‘ALL WILL BE WELL’ – much love from Patricia in Scotland xx
Sitting here in a beautiful cathedral type church here in Linlithgow after a 15 minute service of ‘stillness’ to pray for you Alice: May our Father God Hold you in The Palm of His Hand these hard days ahead, and may you know of His Healing Touch and His Extraordinary Peace and Comfort.
Amen.
It is what it is will now be a statement I’ll be using from now on. Thankyou for sharing your fight, battle, life games with us – you are inspiring many of us without realising it. I have been on the Anthony Nolan Bone Marrow donor list for over 30 years and never been able to help anyone yet. Lots of love from all at Launton Village players xx
Your blog is moving, honest, brave, positive, and inspiring.
Good luck this week.
Please send me a message if there is something you think a stranger can do to help.
Alice,
I don’t know if you remember me as one of the Martin clan (pretty irrelevant), but I just wanted to show my support. I’ve been fighting to write a comment from your first post, because as lovely as they all are and with no intention of offending anyone, they must become repetitive. However, I can’t resist any more…you truly are the biggest inspiration. With a few old memories of being in the same riding group at Fizz’s yard and crossing paths on the playground and Sunday school, I’m bloody proud to say I even know OF you. Your attitude towards every piece of sh*t thrown your way is beyond mind boggling. Amazing. Not to mention your writing skills.
So, I guess I just want to send my love and support to you and your family. I truly mean it. I think about you often and your posts are all inspiring pieces of art. Not that they are to be exhibited, but you must know that what you are doing is incredible and thought provoking to say the least.
Lots of love to you Alice, you are amazing.
Evie X
Alice
Last September I sat beside you in the Churchill Day Unit having my first transfusion. You seems so relaxed and knowledgable about what was happening and you chatted to me about your diagnosis.
Thank you for writing your blog. You are an amazingly gifted writer and a truly inspirational person.
All the very best with your transplant and for sharing your experiences and thoughts.
Alice, you are inspiring. Such a strong person to have the kind of attitude you have at your age in such circumstances. You’ve been dealt a tough hand, but as you say, it is what it is. Fingers crossed for this week and I wish you every success and all the best xx
Hello Alice
I have been reading your blog, and wanted to say hello and good luck for the operation tomorrow. I work at Cancer Research UK, and continue to be inspired by young people like you who are strong, inspiring and optimistic in the face of cancer treatment. Good luck from me and the team here, I am looking forward to reading how things progress.
Alice, your blog is so well-written, and as many others have said, you are incredibly inspiring and the way you are dealing with your situation is truly admirable. Wishing you all the best with everything, and fingers crossed for a positive update. x